
Precedent
AI Demand Generation Stealth Tech The first AI platform built by insurance carrier insiders to automate pre-litigation PI demands
Precedent doesn't show up in our technology scans. There's no JavaScript widget on your website, no DNS record to detect, no pixel firing in the background. It's a closed-loop platform that lives entirely inside the firm's case workflow — ingesting medical records, drafting demands with cited arguments, and delivering them directly to insurance carriers. That makes it invisible to web-based detection, which is exactly why it deserves a dedicated review. The firms using Precedent aren't just adding another tool to their marketing stack — they're fundamentally changing how pre-litigation cases move through the pipeline.
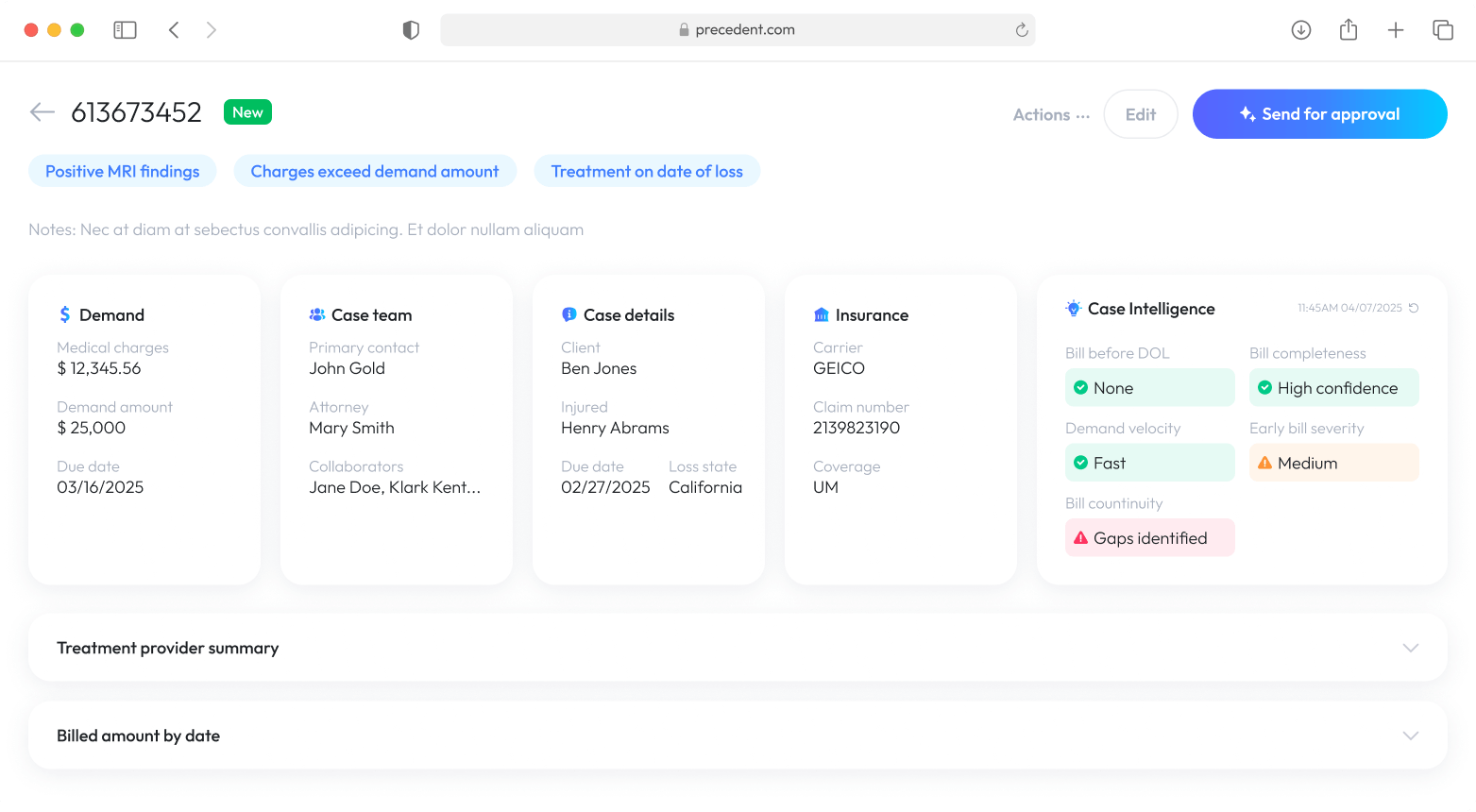 The Precedent case dashboard — demand economics, case team, insurance details, and AI-powered Case Intelligence in one view.
The Precedent case dashboard — demand economics, case team, insurance details, and AI-powered Case Intelligence in one view.
Most "AI legal tech" is a thin wrapper around a large language model with a legal prompt template. Precedent is different. It was built by people who spent their careers on the insurance carrier side — adjusters, claims managers, the people who actually read and evaluate demand letters. That carrier DNA shows up in how the platform structures arguments, calculates damages, and anticipates defense tactics. The result is demand packages that are structured the way adjusters actually process claims, with hyperlinked citations to the exact page in the medical records.
Demand Composer
The flagship product. Upload medical records, bills, and case documents. Precedent's AI reads everything, builds an injury narrative with ICD-10 coded diagnoses, calculates damages with itemized specials and a supported general damages argument, and produces a complete demand letter — typically in hours, not days. Every medical citation hyperlinks back to the source page in the records. The output reads like it was written by a senior paralegal who spent two days on the file.
Case Intelligence
Before you even start drafting, Case Intelligence analyzes the file and flags issues: gaps in treatment, billing continuity problems, missing records, and early severity indicators. It tells you what the adjuster will challenge before you write a single word. This is the feature that separates Precedent from "we generate a demand letter" competitors — it's strategic pre-demand analysis that most firms only get from their most experienced attorneys.
MedChron
Automatically generates medical chronologies from ingested records — every provider visit, treatment, medication, and diagnostic on a navigable timeline with page citations. What used to take a paralegal an entire day takes Precedent minutes, and the output is more complete because the AI doesn't skip entries when it gets tired at 4 PM.
Claim Setup & Policy Verify
Files carrier claims within 48 hours without phone calls, and retrieves policy limits and coverage information. These feel like "boring" features compared to AI demand drafting, but they eliminate two of the biggest bottlenecks in pre-litigation: the week-long wait to confirm coverage, and the intake coordinator spending 45 minutes on hold with GEICO.
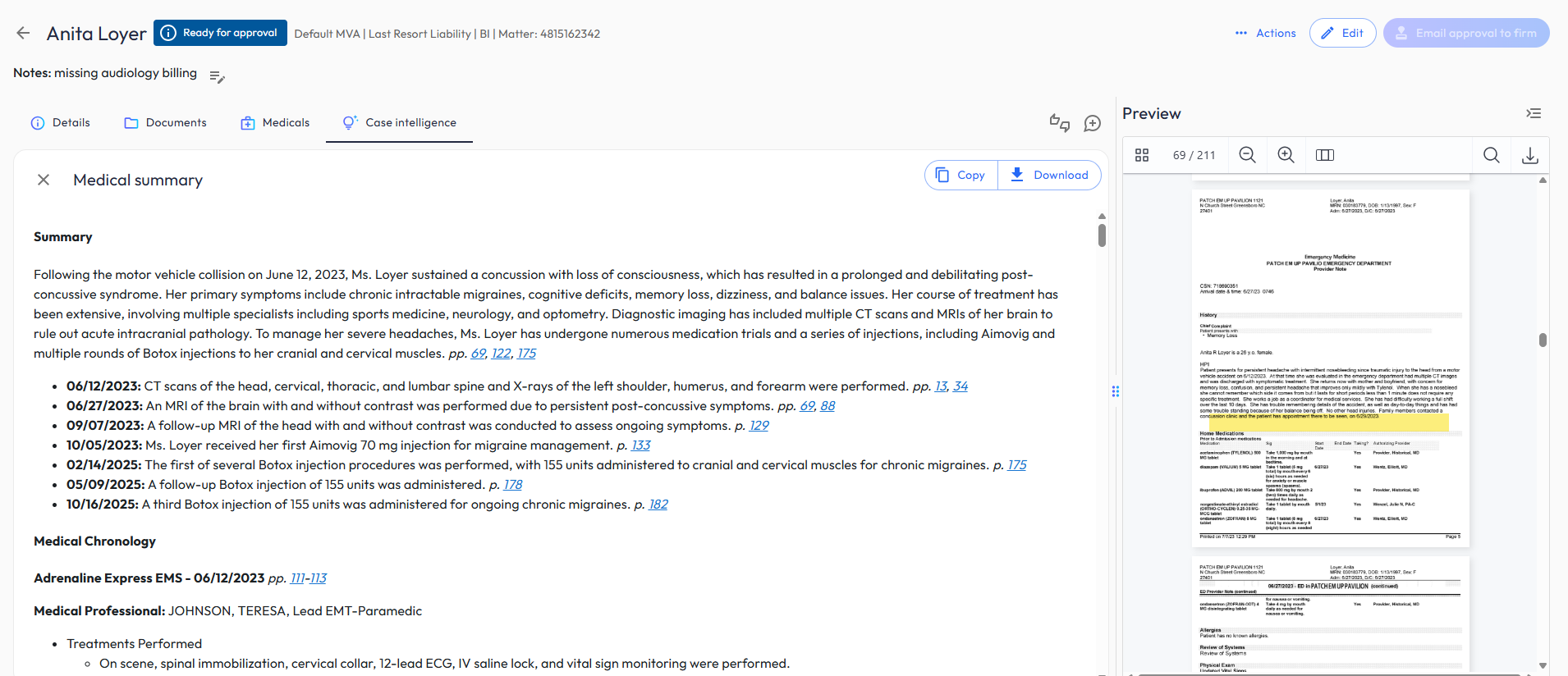 AI-generated medical summary with hyperlinked page citations alongside the original records.
AI-generated medical summary with hyperlinked page citations alongside the original records.
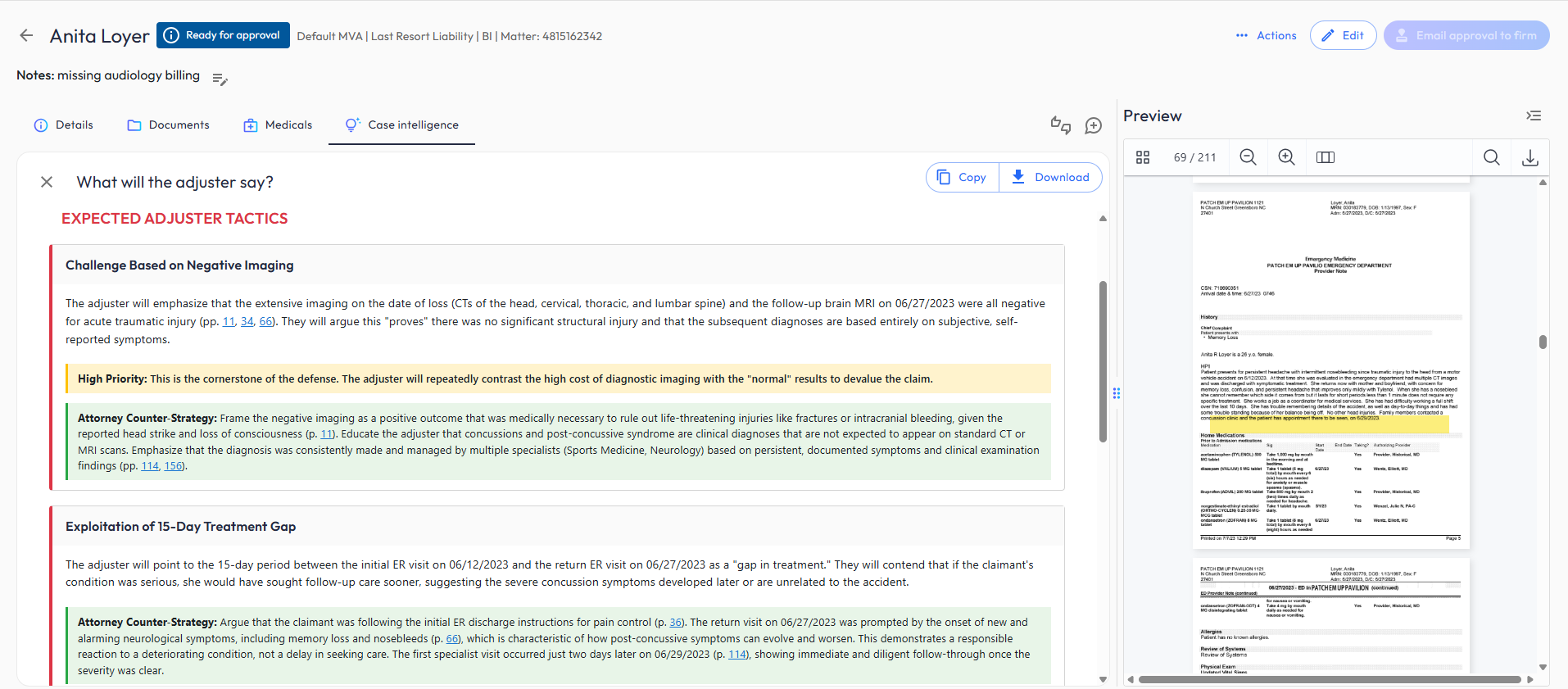 "What will the adjuster say?" — predicted defense tactics with specific counter-strategies.
"What will the adjuster say?" — predicted defense tactics with specific counter-strategies.
This is the part that actually matters and the part most firms overlook when evaluating demand automation tools. Precedent wasn't built by software engineers who read some legal textbooks. It was built by people who spent years inside insurance carriers evaluating claims. They know which arguments adjusters actually respond to, which damage calculation methods get taken seriously, and which formatting patterns trigger the "this is a real demand" response versus the "this is template garbage" response.
The "What will the adjuster say?" feature is the clearest evidence of this. It doesn't just predict generic objections — it identifies the specific vulnerabilities in YOUR case file (treatment gaps, negative imaging, delayed onset) and provides counter-arguments with page citations. This is the kind of strategic thinking that usually requires a senior attorney who's been negotiating with carriers for 15 years.
- Start with your 10 most "average" cases, not your best or worst. Precedent's value is clearest on the $15K-$75K pre-litigation cases that make up the bulk of a PI firm's volume. These are the cases where spending two attorney-days writing a demand letter doesn't pencil out, but sending a weak demand leaves money on the table. Start here, compare settlement amounts to your historical average, and expand from there.
- Upload everything — even documents you think are irrelevant. The AI can't find treatment gaps or billing inconsistencies if it doesn't have the full picture. Police reports, ER discharge instructions, pharmacy records, even the denial letter from the carrier. More context produces significantly better demand narratives and more accurate damage calculations.
- Use Case Intelligence before you decide whether to demand or litigate. The pre-demand analysis often reveals case strengths and weaknesses that change the strategy. A case you thought was a clear $30K demand might have elements that support a $60K demand — or fatal weaknesses that mean you should settle fast rather than invest in a demand package.
- Review and customize the output — don't just send it blind. Precedent learns your firm's voice over time, but the attorney should always review for case-specific nuances the AI might miss: the client's emotional testimony, the surgeon's specific prognosis language, or a jurisdictional quirk. The best results come from attorneys who spend 15 minutes refining what would have taken them 6 hours to draft from scratch.
- Track your before/after metrics religiously. Record your average settlement amount, time-to-tender, and demand-to-settlement ratio for 30 cases before Precedent, then compare after 30 cases with it. The 17% settlement increase they claim is an average — your results will vary by case mix, and having hard data helps you decide whether to expand usage or adjust your workflow.
- EvenUp — The largest player in AI demand generation. However, EvenUp has historically relied on offshore human drafters augmented by AI, not pure AI generation. This means longer turnaround times, higher costs ($500-$800+ per demand), and less consistency. They've been adding more AI automation, but the hybrid model creates a fundamentally different product than Precedent's AI-first approach. EvenUp is better known but not necessarily better.
- Supio — Focuses on medical record analysis and chronology generation rather than full demand drafting. If you're happy with your demand writing process but drowning in medical records, Supio might be the right tool for the specific pain point. It's not a direct Precedent competitor — it's more of a component that overlaps with Precedent's MedChron feature.
- CaseGlide — An older player focused on the carrier side (claims management). Some plaintiff firms use it for case analytics, but it's not built for demand generation. Mentioned here because it sometimes comes up in competitive conversations.
- Doing it yourself with a senior paralegal — For firms handling fewer than 15 pre-lit cases per month, a skilled paralegal with a good template library might be more cost-effective than any platform. The math changes when you're doing 30+ demands per month — that's where the $275 flat rate starts saving serious money versus $50-$75/hour paralegal time over 6-8 hours per demand.
- Use the "What will the adjuster say?" output as deposition prep. If a case goes to litigation, the adjuster objections Precedent predicted — and the counter-arguments it provided — are a roadmap for deposing the adjuster or claims manager. You'll walk in knowing exactly what they'll argue and why it doesn't hold up.
- Run every case through Case Intelligence even if you're not using Demand Composer. The pre-demand analysis is valuable even for cases you plan to litigate. It identifies record gaps, billing issues, and coverage problems early enough to fix them before they become defense ammunition.
- Use Precedent's medical chronologies for client communication. The MedChron output is clear enough for a non-lawyer to follow. Send it to your client with a note: "Here's a summary of your treatment history — please let us know if anything is missing." Clients catch records gaps that AI and paralegals miss because they remember the appointment they had that somehow didn't get documented.
- Compare Precedent's damage calculation to your own before sending. If there's a significant gap between what Precedent calculates and what you would have demanded, figure out why. Sometimes the AI catches damages you'd have missed (future medical, loss of enjoyment). Sometimes you know something the AI doesn't (a client who presents exceptionally well). Either way, the comparison makes the final number stronger.
- Feed the declined-case data back into your intake process. When Case Intelligence flags a case as weak (statute of limitations issues, minimal treatment, disputed liability), that intelligence should flow back to intake. If you're consistently signing cases that Precedent identifies as problematic, your intake screening questions need work.
- No monthly subscription
- No prepaid token packages
- Unlimited revisions included
- First case free (trial)
2025 Clio Integration Awards Finalist for "Best New App." Encrypted data handling with a closed-loop system — medical records and case data never leave the platform's secure environment.
Precedent is one of the few legal AI products that feels like it was built by people who understand the actual problem, not just the technology. The carrier-insider perspective produces demand letters that are structured for how adjusters actually evaluate claims — which is why the settlement numbers move. At $275 per demand with no subscription overhead, the unit economics work for any firm doing meaningful pre-litigation volume. The Case Intelligence and MedChron features alone justify evaluation even if you're not ready to outsource demand drafting.
The biggest risk is the same as any AI legal tool: overreliance. Precedent is a force multiplier for good attorneys, not a replacement for legal judgment. The firms getting the best results are the ones that use it to handle the 80% of mechanical work (record summarization, damage calculation, argument structuring) so their attorneys can focus on the 20% that actually requires human judgment — case strategy, client relationships, and the nuances that algorithms can't capture.
